|
Less than 6 mm is considered normal up to 22 weeks. The nuchal fold is a measurement taken from the outer skin line to the outer bone in the midline. A measurement of 2–10 mm is normal in the second and third trimesters. The cisterna magna can be measured from the posterior margin of the cerebellar vermis to the inside of the occipital bone in the midline. A cerebellum measuring 2 mm less than gestational age is a concerning finding. The trans-cerebellar diameter (the widest measurement across the cerebellum perpendicular to the falx) in millimeters correlates with the gestational age up to 20 weeks and is larger than gestational age after this time. The central vermis is slightly more echogenic than the lateral lobes. The cerebellum is a dumbbell-shaped structure with symmetrical lobes. The plane is correct when one can visualize the thalami and cavum septum pellucidum in the same plane as the cerebellum. Trans-cerebellar plane: This plane is inferior to the BPD plane, with the probe tilted backward into the posterior fossa. This unequivocal demand of carefulness is best expressed by the ALARA principle (i.e., as low as reasonably achievable). Exposure time and acoustic output should be kept to the lowest levels consistent with obtaining diagnostic information and limited to medically indicated procedures, rather than purely entertainment purposes. This should not prevent the use of this mode when clinically indicated, provided the user has adequate knowledge of the instrument’s acoustic output or has access to the relevant TI. The significant temperature increase may be generated by spectral Doppler mode, particularly in the vicinity of a bone. 
Both indexes are not perfect indicators of the risks of thermal and non-thermal bioeffects, but currently, they should be accepted as the most practical and understandable methods of estimating the potential for such risks.Īcoustic outputs in B-mode and M-mode are generally not high enough to produce deleterious effects. American Institute of Ultrasound in Medicine (AIUM) and National Electrical Manufacturers Association (NEMA) regulated that the ultrasound device has to display the emitted energy through the thermal index (TI) and the mechanical index (MI). īased on evidence currently available, routine clinical scanning of every woman during pregnancy using real-time B-mode imaging is not contraindicated. On the other hand, in low-risk pregnant women, the scan could also be sensitive in anomaly detection if a systemic searching pattern was followed. 
The detection rate of the screening second-trimester ultrasound scan was good in high-risk patients examined by the well-trained sonographer. The literature includes descriptions of anatomical surveys performed before 18 weeks, but other studies have repeatedly shown that more anomalies are diagnosed if the scan is done after 18 weeks. A normal scan is often obtained, but there is tremendous relief of psychological distress, anxiety, and somatic symptoms after the report. 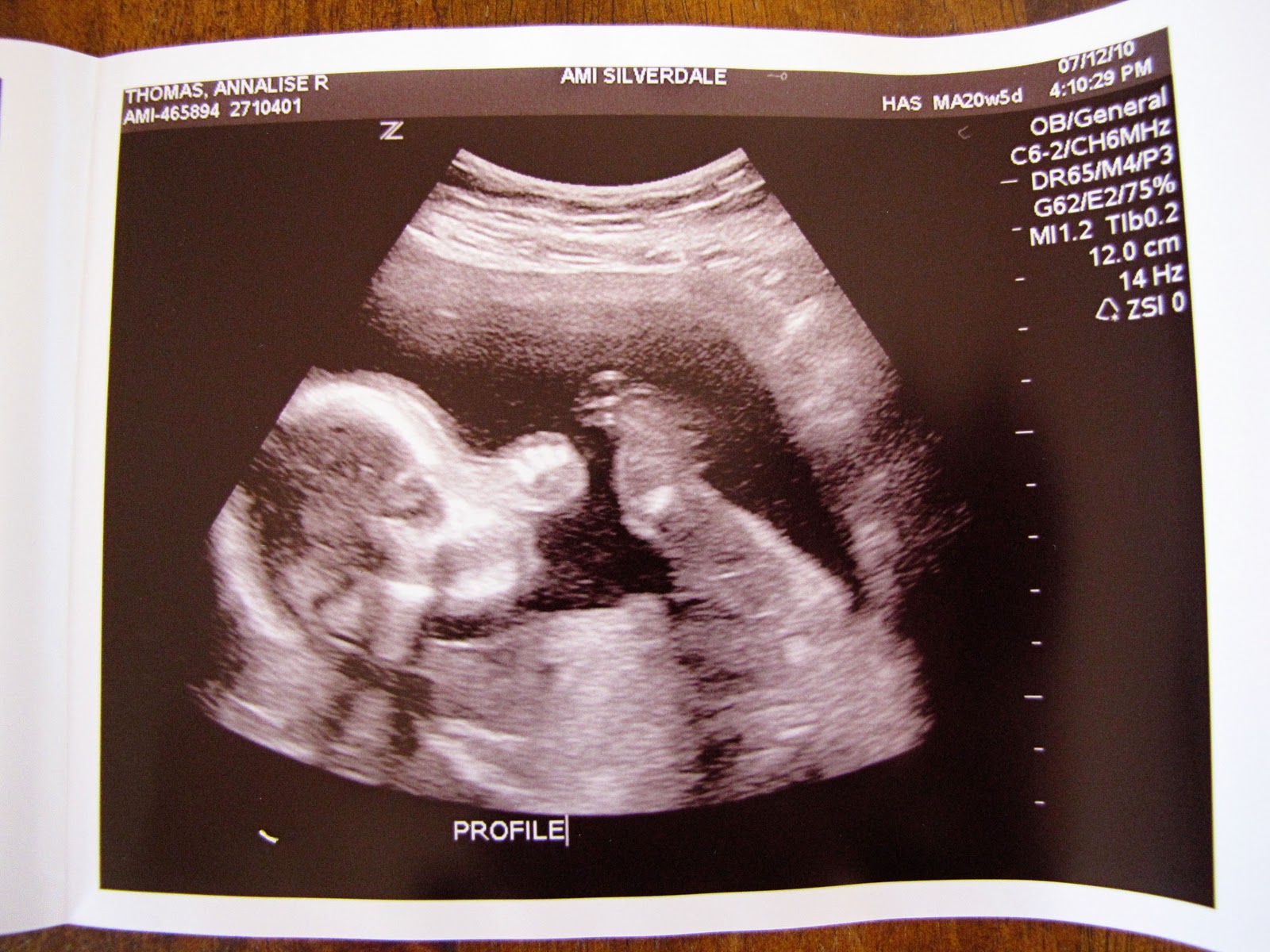 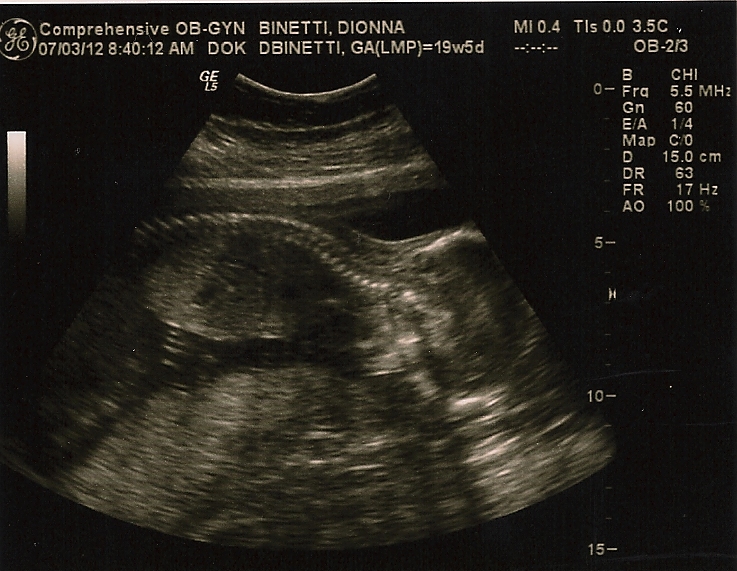
Performed systematically, high-resolution ultrasound can now accurately diagnose more than 200 abnormalities. It thereby decreases the probable complications of continuation of pregnancy and labor, prevent an unnecessary cesarean section for a fetus with lethal anomalies diagnosed too late for medical termination of pregnancy, and allow planning delivery at the optimal time in a well-equipped tertiary center with necessary neonatal care facilities, and in utero therapy in selected cases. Prenatal diagnosis enables a psychologically less traumatic and early medical termination of pregnancy. The diagnosis of a fetal anomaly significantly reduces perinatal mortality and morbidity and maternal morbidity. Clinical researchers have seized technological developments such as real-time imaging, color, and power Doppler, transvaginal sonography, and 3/4D imaging to enhance the investigation and management of patients in areas as diverse as assessment of fetal growth and wellbeing, screening for fetal anomalies, and ultrasound-guided procedures as an essential component of fetal therapy. The history of sonography in Obstetrics dates from the classic 1958 Lancet paper of Ian Donald and his team from Glasgow. Although ultrasound screening is now an integral part of routine antenatal care, recommendations for the delivery of obstetric ultrasound vary from country to country. Antenatal ultrasonography is widely used in pregnancy to assess fetal growth and anatomy.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
